Chronic lymphedema is considered a progressive condition, regardless of whether it is classified as primary or secondary, and cannot simply be described as an accumulation of protein-rich fluid. It is a chronic degenerative and inflammatory process affecting the soft tissues, skin, lymph vessels, and nodes, and may result in severe and often disabling swelling.
Lymphedema may present in the extremities, trunk, abdomen, head and neck and external genitalia and can develop anytime during the course of a lifetime in primary cases; secondary cases may occur immediately following the surgical procedure or trauma, within a few months, a couple of years, or twenty years or more after treatment.
Lymphedema progresses through stages, and treatment intervention in early stages (stage 0 and stage I) has been shown to result in very good treatment outcomes if managed appropriately (1).
There are four stages of lymphedema
Click here for a short video explaining the stages of lymphedema
Stage 0, also known as latent stage or subclinical stage of lymphedema
In this stage the transport capacity of the lymphatic system is reduced, but the remaining lymph vessels are sufficient to manage the flow of lymph, and swelling is not visibly present.
Examples include individuals who underwent surgeries for malignancies, such as breast cancer, cancer affecting the genitourinary and gynecologic systems, cancers in the head and neck region, melanoma or soft tissue malignancies. These procedures generally include the removal of lymph nodes with subsequent disruption of lymphatic pathways.
A condition known as lymphangiopathy is present if the reduction in the transport capacity of the lymphatic system is caused by pathology affecting the lymphatic system directly in form of a developmental abnormality (malformations, as in primary lymphedema). In this case lymphedema is not clinically present as long as the lymphatic system is able to cope.
In stage 0 patients may experience early symptoms, such as the feeling of numbness, tingling or fullness in a limb, which is often accompanied by low-grade discomfort. It may be difficult to fit into clothing, and watches, rings or bracelets may feel tight. This subclinical stage can exist for months, or years, before any more serious signs appear. The onset of lymphedema correlates to the ability of the lymphatic system to compensate for the reduced transport capacity and any added stress to the system that may cause an increase in the volume of lymphatic fluid.
Early diagnosis and appropriate treatment of lymphedema is of paramount importance to limit progression of the swelling and to avoid complications often associated with untreated or incorrectly treated lymphedema; several studies have shown that patients’ self-reported symptoms are very accurate indicators of early lymphedema. While subclinical lymphedema can be detected using methods such as bioimpedance (2) and perometry (3), these technologies are not yet widely available.
Treatment intervention in this early and easily manageable stage has been shown to result in very good treatment outcomes using simple, non-custom compression garments (4).
Stage I, also known as pitting or reversible stage
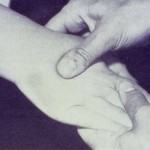 Body parts such as the arms or legs are visibly swollen as protein-rich fluid starts to accumulate in the tissues. In many cases, the swelling subsides with elevation and the limb may appear normal in the morning; however, as soon as the limb is in a dependent position, the swelling returns. Pitting is easily induced by pressing with the thumb, and the indentation produced by this pressure is retained for some time.
Body parts such as the arms or legs are visibly swollen as protein-rich fluid starts to accumulate in the tissues. In many cases, the swelling subsides with elevation and the limb may appear normal in the morning; however, as soon as the limb is in a dependent position, the swelling returns. Pitting is easily induced by pressing with the thumb, and the indentation produced by this pressure is retained for some time.
 While an increase in proliferating cells (increase in fibrous connective tissue) may be present, this early stage lymphedema is considered reversible because the skin and tissues have not yet been permanently damaged. With proper management it is possible for the patient to expect reduction of the extremity to a normal size (compared with the uninvolved limb). Without proper treatment, progression to the next stage is unavoidable in the vast majority of the cases.
While an increase in proliferating cells (increase in fibrous connective tissue) may be present, this early stage lymphedema is considered reversible because the skin and tissues have not yet been permanently damaged. With proper management it is possible for the patient to expect reduction of the extremity to a normal size (compared with the uninvolved limb). Without proper treatment, progression to the next stage is unavoidable in the vast majority of the cases.
Stage II, also known as spontaneously-irreversible stage
 It is important to point out that the stage of lymphedema is not defined by size, but rather by the consistency of the tissues. This stage is primarily identified by tissue proliferation with subsequent thickening and hardening of the soft tissues. In many cases the swelling increases and elevation of the limb rarely reduces the swelling; pitting is evident. Over time, the tissue continues to harden and excess fatty tissue begins to form and pitting becomes difficult to induce.
It is important to point out that the stage of lymphedema is not defined by size, but rather by the consistency of the tissues. This stage is primarily identified by tissue proliferation with subsequent thickening and hardening of the soft tissues. In many cases the swelling increases and elevation of the limb rarely reduces the swelling; pitting is evident. Over time, the tissue continues to harden and excess fatty tissue begins to form and pitting becomes difficult to induce.
A reduction in volume can be expected if proper treatment is initiated in this stage. In most cases, the excess fibrotic tissue typical in this stage will not recede during the intensive phase of complete decongestive therapy (CDT). Reduction in tissue fibrosis is mainly achieved in the second phase of CDT with proper compression and good patient compliance.
Stage III, also known as lymphostatic elephantiasis
Lymphedema often stabilizes in stage II. However, if lymphedema remains untreated, protein-rich fluid continues to accumulate, leading to further 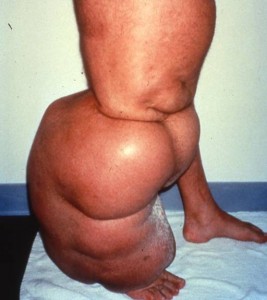 increase of swelling, sometimes resulting in extreme proportions. Hardening of the tissue continues and further deposition of fat it present. In this state, pitting is absent and the swollen body part becomes a perfect culture medium for bacteria and subsequent recurrent infections (lymphangitis) are frequent. Moreover, untreated lymphedema can lead into a decrease or loss of functioning of the affected extremity, skin breakdown and sometimes irreversible complications.
increase of swelling, sometimes resulting in extreme proportions. Hardening of the tissue continues and further deposition of fat it present. In this state, pitting is absent and the swollen body part becomes a perfect culture medium for bacteria and subsequent recurrent infections (lymphangitis) are frequent. Moreover, untreated lymphedema can lead into a decrease or loss of functioning of the affected extremity, skin breakdown and sometimes irreversible complications.
Reduction can still be expected if treatment starts in this stage. In most cases the duration of the intensive phase of complete decongestive therapy has to be extended and repeated several times. In extreme cases the surgical removal of excess skin following the conservative therapy may be indicated (5).
Dear Lymphedema Blog Reader – if you like the contents on this website, please help to keep it going. A great amount of work and research is necessary to provide you with up-to-date information on this site. Your donation supports these efforts and associated administrative costs. Surplus funds will be donated to Lymphedema/Lipedema-related charitable endeavors. Please donate using the “Donate Now” button on the right upper hand of this page – Thank You!
Join Lymphedema Guru, a Facebook page solely dedicated to inform about all things related to lymphedema – news, support groups, treatment centers, and much more
1. Torres Lacompa, M, Yuse Sanches, MJ, et al.(2010) Effectiveness of early physiotherapy to prevent lymphedema after surgery for breast cancer: randomized, single blinded, clinical trial, BMJ, 340:b5397.


 Joachim Zuther, Lymphedema Specialist.
Joachim Zuther, Lymphedema Specialist.