While secondary lymphedema is caused by blockage or damage to a normally functioning lymphatic system resulting from surgery, radiation, trauma and other known insults, the formation of primary lymphedema is caused by pathology affecting the structure and function of the lymphatic system directly in form of a developmental abnormality, most commonly hypoplasia or hyperplasia involving lymph vessels and/or lymph nodes.
Hypoplasia, the most common malformation, refers to an incomplete development, that is, the number of lymph vessels and/or nodes is reduced, or the size of these lymphatic structures is smaller than normal.
Hyperplasia is generally associated with a structural malformation of lymph vessels and/or nodes (lymphangiectasia, or megalymphatics); enlargement (dilation) of lymph vessels in this case may result in a malfunction of valves located within the lymph collectors, compromising the flow of lymphatic fluid.
Lymphatic aplasia is rare and describes the absence of single lymph vessels and/or nodes, which may be the cause for the onset of primary lymphedema.
Primary lymphedema is far less common than the secondary form; it has been estimated to affect 1 in 100,000 people worldwide (1,5), predominantly in female patients with a ratio of one male to three females. In the majority of primary lymphedema cases, the lower extremities are affected.
Click here for a short video on the incidence of primary lymphedema
The maldevelopment of the lymphatic system in primary lymphedema is inherited, which means it can pass from generation to generation.
Several genes (VEGFR3, FOXC2, SOX18, ANGPT2, others) can be involved in the development of the lymphatic system (2) and mutations of any of these genes may cause lymphedema. However, only one of these genes is typically responsible for the lymphatic malformation in a particular family. Inherited lymphedema presents in an autosomal dominant pattern with incomplete penetrance and variable expression.
Primary lymphedema can also be associated with a known syndrome (Turner, Noonan, Hennekam, others).
What does that mean?
Except for genes on the sex chromosomes, both males and females have two copies of each gene. If only one altered copy of a gene (mutation) causes a malformation, the condition will be inherited in what is called a dominant pattern, which essentially means that children of parents with primary lymphedema have a 50% chance of inheriting the defective gene. This, however, does not explain why primary lymphedema is more common in female offspring; further studies will hopefully shed more light on this phenomenon.
 In genetics the strength of a gene is described as penetrance; a strong penetrance is present if all children who inherit the abnormal gene develop primary lymphedema. If only a fraction of children who inherit the abnormal gene actually develop the condition, the penetrance is described as inconsistent or variable. This is the case with the lymphedema gene; not all children who inherit the mutation will show evidence of lymphedema. In many cases of primary lymphedema it can be established that the condition skipped one or more generations.
In genetics the strength of a gene is described as penetrance; a strong penetrance is present if all children who inherit the abnormal gene develop primary lymphedema. If only a fraction of children who inherit the abnormal gene actually develop the condition, the penetrance is described as inconsistent or variable. This is the case with the lymphedema gene; not all children who inherit the mutation will show evidence of lymphedema. In many cases of primary lymphedema it can be established that the condition skipped one or more generations.
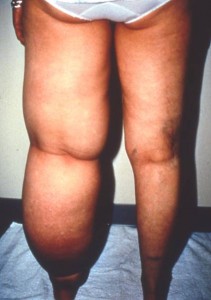
Variable expression indicates that the swelling may affect the left leg of one family member, another family member’s right foot, and yet another family member may have both legs involved.
In addition, the age of presentation can also be quite variable. Although the abnormalities in the development of the lymphatic system are present at birth, lymphedema may develop at any point later in life, most often during puberty or pregnancy with a peak in the onset between the ages 10 and 25. However, primary lymphedema may not visibly develop at all as long as the genetically compromised lymphatic system is sufficient enough to manage its workload.
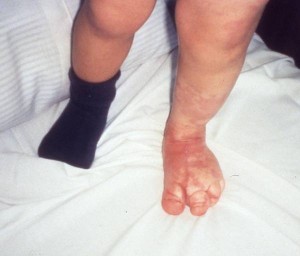 Primary lymphedema can be classified by the age of the patient at the onset of the swelling. Congenital (pediatric) lymphedema is present at birth or within the first two years of life and accounts for 10-25% of all cases of primary lymphedema. Boys typically are affected at birth, and girls most often present with lymphedema during adolescence (3). A sub-group of patients with congenital lymphedema has a familial pattern of inheritance, which is known as Milroy’s disease (VEGFR3 mutation) (4).
Primary lymphedema can be classified by the age of the patient at the onset of the swelling. Congenital (pediatric) lymphedema is present at birth or within the first two years of life and accounts for 10-25% of all cases of primary lymphedema. Boys typically are affected at birth, and girls most often present with lymphedema during adolescence (3). A sub-group of patients with congenital lymphedema has a familial pattern of inheritance, which is known as Milroy’s disease (VEGFR3 mutation) (4).
The most common form of primary lymphedema is termed lymphedema praecox, also known as Meige’s disease (no known gene mutation); by definition, it becomes clinically evident after birth and before age 35. This condition accounts for 65-80% of all primary lymphedema cases and most often arises during puberty or pregnancy.
A relatively rare form of primary lymphedema is when the first signs of swelling appear after 35 years of age; this condition is called lymphedema tarda.
Regardless of the cause, there is no cure for lymphedema. However, primary lymphedema can be very effectively managed, especially if it is diagnosed early. Individuals affected by lymphedema may encounter a number of problems, which can be either attributed to other pathologies (comorbidities) that may be present in addition to existing lymphedema and further exacerbate its symptoms, or secondary complications which may develop as a result of stagnated lymphatic fluid. Secondary complications are common to lymphedema, especially if the swelling is left untreated, and often contribute to the progression of the swelling.
Both early diagnosis and intervention of lymphedema are equally crucial for optimal treatment results. Whether lymphedema is caused by developmental abnormalities, or surgery/radiation to the lymphatic system, the possible long-term physical and psychosocial burden resulting from untreated or mistreated lymphedema can be serious.
Proper treatment is available, and the classification of lymphedema into primary and secondary has little significance in determining the method and goal of therapy. The goal of any treatment is to reduce the swelling and to maintain the reduction – that is to bring the lymphedema back to a normal, or near-normal size so affected individuals can continue with the activities of daily living, and to limit the risk of infection.
 The accepted gold-standard for the treatment of lymphedema is Complete Decongestive Therapy (CDT). Backed by long standing experience this therapy has shown to be safe and effective as the standard therapy for lymphedema. Click here to read more about CDT.
The accepted gold-standard for the treatment of lymphedema is Complete Decongestive Therapy (CDT). Backed by long standing experience this therapy has shown to be safe and effective as the standard therapy for lymphedema. Click here to read more about CDT.
Recent developments in research indicate that drugs are beginning to become available to oppose or correct the effects of gene mutations (6, 7).
Dear Lymphedema Blog Reader – if you like the contents on this website, please help to keep it going. A great amount of work and research is necessary to provide you with up-to-date information on this site. Your donation supports these efforts and associated administrative costs. Surplus funds will be donated to Lymphedema/Lipedema-related charitable endeavors. Please donate using the “Donate Now” button on the right upper hand of this page – Thank You!
Join Lymphedema Guru, a Facebook page solely dedicated to informing about all things related to lymphedema – news, support groups, treatment centers, and much more
References:
- http://jmg.bmj.com/content/22/4/274.full.pdf
- https://pubmed.ncbi.nlm.nih.gov/18564921/
- http://www.ncbi.nlm.nih.gov/pubmed/21617474
- http://ghr.nlm.nih.gov/condition/milroy-disease
- https://www.frontiersin.org/articles/10.3389/fphys.2020.00137/full
- https://pubmed.ncbi.nlm.nih.gov/34112235/
- https://pubmed.ncbi.nlm.nih.gov/29461977/
Video:
Primary Lymphedema: How Science Has Changed Patient Care – Dr. Peter Mortimer
Further Reading:
http://www.lymphnet.org/pdfDocs/nlntreatment.pdf
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC1287178/
http://www.ncbi.nlm.nih.gov/pubmed/9817924
http://adc.bmj.com/content/71/1/44.full.pdf
http://plasticsurgerynotes.net/Lower_Extrimity/lymphatic_disorders.asp
http://www.hgen.pitt.edu/projects/lymph/inheritance.php
http://emedicine.medscape.com/article/191350-overview#a0102
http://www.lymphedemapeople.com/thesite/primary_lymphedema.htm
http://www.medicinenet.com/lymphedema/article.htm
http://www.noblemed.com/primary.htm
http://www.ncbi.nlm.nih.gov/pubmed/18564921y
http://www.ncbi.nlm.nih.gov/pubmed/6843174


 Joachim Zuther, Lymphedema Specialist.
Joachim Zuther, Lymphedema Specialist.