Taking appropriate precautions to reduce the risk of developing lymphedema always makes sense. Traveling in airplanes with pressurized cabins at high altitudes, especially on long-haul flights, may have deleterious effects on unmanaged lymphedema. However, individuals affected by, or at risk for lymphedema should not avoid air travel due to fear. Being aware of the possible physical stresses on the body during air travel is important and enables patients to take appropriate precautions.
Recently, some studies have been published that suggest flying doesn’t seem to increase the risk of increased swelling or the onset of lymphedema in patients at risk, however, there are many studies that suggest otherwise. While more research is needed, common sense suggests minimizing the risks whenever possible.
This article addresses suggestions to help reduce the risk of triggering lymphedema and prevent existing lymphedema from progressing during and after airline travel.
A Short Primer on Lymphedema:
The onset of lymphedema is caused by a reduced transport capacity of the lymphatic system resulting in the inability to respond to an increase of lymphatic loads. This causes water and protein to accumulate in the tissues, which may result in chronic alterations and infections if left untreated.
Lymphedema can be defined as high-protein edema and is classified as either primary or secondary; lymphedema may be mild, moderate or severe, affects most often the extremities but may also be present in other parts of the body.
In primary lymphedema the transport capacity is reduced as a result of a developmental abnormality of the lymphatic system. Primary lymphedema may be present at birth, but more often develops later in life with or without obvious cause.
Secondary lymphedema is more common and is caused by surgical interventions involving the lymphatic system. Lymph node dissections, radiation therapy or incisions disrupting the natural pathways of the lymphatic system affects its ability to drain lymphatic loads out of the affected extremity. Secondary lymphedema may arise immediately after surgery or not develop for years.
Chronic venous insufficiencies, infections involving the lymphatic system, trauma, or malignancies affecting the lymphatic system either from the inside or exerting pressure from the outside, may be other causes for the onset of secondary lymphedema.
Lymphedema may be reduced to a normal or near normal size if proper treatment techniques are utilized. However, once lymphedema is present, the lymphatics are never normal again and the affected body part is always at risk of developing more lymphedema.
Effects of Altitude on Air Pressure:
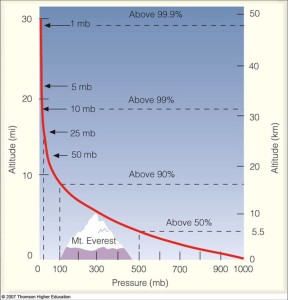 The air’s pressure is caused by the weight of the air pressing down on the earth, the body, and the ocean as well as on the air below. The pressure value depends on the amount of air above the point where the pressure is measured; if altitude increases, the pressure falls. The exact pressure at a particular altitude depends on weather conditions. To understand the general idea of how pressure decreases with altitude the following approximation can be used:
The air’s pressure is caused by the weight of the air pressing down on the earth, the body, and the ocean as well as on the air below. The pressure value depends on the amount of air above the point where the pressure is measured; if altitude increases, the pressure falls. The exact pressure at a particular altitude depends on weather conditions. To understand the general idea of how pressure decreases with altitude the following approximation can be used:
As a rule of thumb, the air pressure drops about 1 inch of mercury for each 1,000-foot increase in altitude or about 0.49 pounds per square inch (psi). At sea level the atmosphere weighs in at about 14.7 psi (101.325 kilopascal or millibar) the pressure of the atmosphere at 8,000 feet is around 10.9 psi (75.156 kilopascal) (1).
Cabin Pressure (Cabin Altitude)
Commercial aircraft are capable of flying at altitudes that are incompatible with human life and yet the passengers and crew are generally not negatively affected because of the on-board environmental and pressurization systems (4). The cabins of aircraft traveling at high elevations are pressurized and the pressure inside the aircraft has to be kept within the design limits of the fuselage. Although pressurized, the cabin pressure is less than that on the ground while traveling at altitude. The cabin pressure of an aircraft intending to cruise at 40,000 feet is designed to rise gradually from the altitude of the airport of origin to around a maximum of 8,000 feet, and to then reduce gently during descent until it matches the air pressure of the destination airport.
Although a cabin altitude of 8000 ft will not pose major health hazards, the decreased cabin pressure can result in lymphedema secondary to the pressure difference.
Regulations (2) require that commercial aircraft be capable of maintaining a cabin altitude no higher than 8,000 feet at the maximum authorized flight altitude; on most flights the cabin pressure is maintained at around 7,000-8000 feet when cruising at 40,000 feet. In other words, while flying at that altitude the atmosphere within the aircraft is like that on a 7,000-foot mountain peak. Referring to the information above, it is apparent that air pressure (and density) at 7,000 feet is lower than on sea level.
Cabin Pressure and the Effects on Lymphedema:
Many patients report that their extremities had started to swell during air travel (3). The most reasonable explanation for this may be inactivity during flight, especially in cases affecting the lower extremities.
Most aircraft are crowded, and passengers are frequently uncomfortable and unable to stretch or easily leave their seats; even people with an intact lymphatic system may develop swollen feet and ankles during long flights. Inactivity in combination with a compromised lymphatic drainage can have even more serious consequences.
Inactivity, with the legs in a downward position coupled with the subsequent pooling of venous blood will lead to an increase in tissue fluid in the lower extremities. This may be enough to trigger the onset of lymphedema in those patients with latent lymphedema (stage 0) or worsen already existing lymphedema in the legs.
In addition to inactivity, other factors may play a crucial role in those patients traveling with lymphedema.
The reduced pressure does have certain effects on those tissues that are or may be affected by lymphedema (suprafascial tissues). Those effects may allow more fluid to be filtered from the blood capillaries into the tissues, some of this fluid must be removed by the lymphatic system. An increase in the interstitial fluid content as a result of increased filtration may be just enough to trigger the onset of lymphedema in individuals with compromised lymphatic drainage (latency stages) or increase the swelling in individuals affected by upper and/or lower extremity lymphedema. It can also be assumed (3) that the lower pressure in cabins allows fibrotic capsules in the tissue to become rounded, causing compression and/or distortion of adjacent structures, such as lymphatic collectors and inlet valves of lymph capillaries. This may also result in increased swelling and/or impeded uptake of lymphatic fluid.
In many cases the elastic fibers in the skin are damaged in lymphedema due to the constant stretch caused by the swelling. This may present an additional factor in the worsening of lymphedema under low cabin pressure environment.
Ways to Avoid the Onset of Swelling during Flight:
Compression therapy seems to be the most effective measure to counter possible negative effects on lymphedema during air travel. Compression therapy (bandages and/or compression garments) increases the pressure within the tissues. This increase in tissue pressure effectively reduces the accumulation of fluid in the tissues and promotes lymphatic and venous return.
It is highly recommended to perform in-flight exercises. Airlines generally provide a pamphlet or video presentation on in-flight exercises, which are especially beneficial if they are performed while wearing compression bandage or garment.
Useful Tips for the Airline Traveler:
Plan ahead:
1. Seek the advice of your physician and your lymphedema therapist if there are any questions.
2. Carry your medication with you. If your destination is located in hot or mosquito-infested areas take precaution (sun screen, insect repellants, and antibiotics).
3. Bring your skin lotion; the air in pressurized cabins is extremely dry.
4. If possible request an exit seat, which gives you more legroom. Definitely request an aisle seat so you can get up periodically without disturbing the person sitting next to you.
5. Allow ample time to check in and reach your departure gate.
6. Wear loose, comfortable clothing and comfortable shoes that have been worn previously. If you have lymphedema of the leg do not take off your shoes during the flight.
7. Make sure that you can manage your luggage. If you travel with another person or a group ask someone else to carry the luggage for you. Should you travel on your own, take a smaller suitcase (preferably one with wheels). Don’t lift your luggage from the baggage carousel with your swollen arm.
8. Check the quality of your compression garment. If you have more than one garment, take the extra one with you as a back up. Remember, if your destination is located at high altitudes you need to take the same precautions as for your flight. Take extra bandages (short-stretch) with you.
Inflight:
1. Relax and enjoy your flight.
2. Eat lightly.
3. Drink plenty of water or fruit juices.
4. Do not place anything under the seat in front of you so you can stretch and exercise your legs.
5. Stand up and walk around the cabin periodically – make sure to observe the fasten seat belt light.
6. Ask somebody else to place your carry-on luggage in the overhead compartment.
7. Make sure to perform some easy to remember “muscle pump” exercises (roll your feet; lift the heels and toes alternating, etc.). Ask your therapist about recommended exercises during the flight.
8. Elevate your arms as often as possible if you have upper extremity lymphedema.
9. Wear your compression garments!
• If you have a stocking with an open toe you may apply bandages on your toes and any other part of your foot that may be exposed.
• It is necessary to wear a glove in addition to your arm sleeve. If you have a gauntlet without finger stubs, you should bandage your fingers.
• It is also a good idea to wear an additional short-stretch bandage on top of your garment to counter the effects of low cabin pressure – talk to your therapist!
Arrival:
1. Do not remove your garment and any additional bandage materials before you reach your final destination.
2. Upon arrival at your hotel, etc. a rest should be your top priority. Make sure to have your limb elevated. A few more exercises with your garments in place would be beneficial.
In addition to the information above, please keep in mind weather you are at home or on vacation all the usual precautions your therapist taught you still apply (you may also visit the National Lymphedema Networks website at www.lymphnet.org to read up on the “Risk Reduction Practices” for upper and lower extremity lymphedema).
Dear Lymphedema Blog Reader – if you like the contents on this website, please help to keep it going. A great amount of work and research is necessary to provide you with up-to-date information on this site. Your donation supports these efforts and associated administrative costs. Surplus funds will be donated to Lymphedema/Lipedema-related charitable endeavors. Please donate using the “Donate Now” button on the right upper hand of this page – Thank You!
Join Lymphedema Guru, a Facebook page solely dedicated to inform about all things related to lymphedema – news, support groups, treatment centers, and much more
Literature:
1: Linda D. Pendleton: Staying Alive; AOPA Pilot Oct. 2002, Vol. 45 No. 10 pages 121-122
2: Electronic Code of Federal Regulations 14 CFR, Chapter 1, Part 25, Section 25-831
3: JR & J Casley-Smith: Lymphedema Initiated by Aircraft Flight; The Journal of Aviation, Space and
Environmental Medicine. Vol 67, No 1; Jan 1996. Lymphedema initiated by aircraft flights – PubMed (nih.gov)
4: Niren L. Nagda and Michael D. Koontz: Review of Studies on Flight Attendant Health and
Comfort in Airliner Cabins; The Journal of Aviation, Space and Environmental Medicine 2003;74:101-9


 Joachim Zuther, Lymphedema Specialist.
Joachim Zuther, Lymphedema Specialist. 
