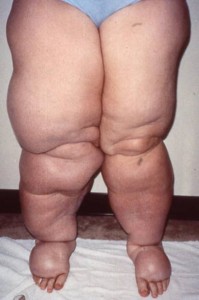
Lipedema is characterized by symmetric enlargement of the limbs, generally affecting the lower extremities extending from the hips to the ankles secondary to the deposition of fat; upper extremities are affected in 30% (1) of the cases.
Lipedema is not rare and not caused by a disorder of the lymphatic system, but is commonly misdiagnosed as bilateral lymphedema, extreme cellulitis, or morbid obesity.
Most commonly used synonyms for lipedema include:
- Adiposalgia/Adipoalgesia
- Adiposis dolorosa
- Lipalgia
- Lipomatosis dolorosa of the legs
- Lipodystrophia dolorosa
- Painful column leg
This condition almost exclusively affects women; according to an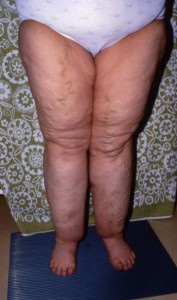 epidemiologic study by Földi E. and Földi M.(2), lipedema affects 11% of the female population, and literature suggests that lipedema is associated with extensive hormonal disorders or liver dysfunctions if present in males.
epidemiologic study by Földi E. and Földi M.(2), lipedema affects 11% of the female population, and literature suggests that lipedema is associated with extensive hormonal disorders or liver dysfunctions if present in males.
Lipedema is a painful fat disorder and if left untreated can cause multiple secondary health problems, to include mobility issues and lymphedema. The quality of life, emotionally and physically, for individuals affected by lipedema is often decreased due to the fact that the condition is typically dismissed as simple obesity by clinicians unfamiliar with the symptoms.
The underlying cause for the development of lipedema remains unknown; it is thought to be associated with hormonal disorders and can be hereditary with 14% of affected individuals having a family history of lipedema (3). Lipedema can develop early in puberty; however, the mean age of diagnosis is approximately 35.
Lipedema can be diagnosed based on clinical criteria (history, typical clinical features) and by physical examination rather than with diagnostic tests.
Clinical Features:
- Symmetrical distribution of fat between the hips and ankles, the feet are
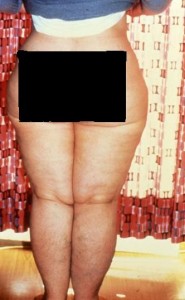 not involved
not involved - Ring of fatty tissue overlapping the tops of the feet
- Tissue has a soft rubber-like feel in early stages
- Initially, the skin color is normal
- Typical bulges of fatty tissue on the medial thigh (above the knee and close to the groin) are seen in later stages
- Small fatty lumps (nodules) within the tissues start to form in later stages
- In the early stages of lipedema the upper part of the body may be slender
- Weight loss does not have an effect on the areas affected by lipedema
- Swelling (edema) is common in the second half of the day and includes the feet but decreases in the early stage with elevation and night-time rest.
- Pain, tenderness, sensitivity to pressure
- Easy bruising
The additional swelling that develops in the later hours of the day in lipedema is of particular interest and is indicative for the involvement of the lymphatic system if lipedema remains without proper management.
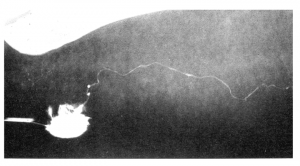
The excessive amount of fatty tissue present in lipedema compresses the lymph collectors of the superficial lymphatic system, which are embedded in the fatty subcutaneous tissue. Lymphangiographic imaging shows that the lymph collectors within the proliferated fatty tissue have a coiled or corkscrew-like appearance rather than passing fairly straight towards the lymph nodes as is the case in healthy tissue. This can result in a reduced transport capacity of the lymphatic system in the affected area.
If the capacity of the lymphatic system is reduced to such an extent that it becomes unable to perform one of its basic functions, the removal of water from the tissues, fluid will accumulate and “real” edema develops in addition to lipedema.
In the initial stages the swelling may recede with elevation and rest, but over time and without adequate treatment (compression, elevation, exercise), the constant strain on the lymphatic system may cause damage to the lymphatic vessels, leading to further reduction of its transport capacity, and swelling may be constantly present.
As a result of prolonged overstrain of the lymphatic system, lymphedema may develop secondary to lipedema (lipo-lymphedema), thereby increasing the complexity of treatment. If lipo-lymphedema remains without treatment, it will progress through the same stages as primary or secondary lymphedema.
Treatment
Active treatment for lipedema is necessary; early diagnosis and treatment can determine long-term prognosis. Therapy for lipedema can be largely divided into conservative treatments to reduce edema, and surgical treatments such as liposuction.
Main goals in the conservative treatment of lipedema are to decrease pain and hypersensitivity, increase mobility and to prevent, or if already present, to address the edematous component associated with lipedema. If lipedema, or lipo-lymphedema is associated with obesity, nutritional guidance must be provided to reduce weight and avoid further weight gain.
Conservative approaches include complete decongestive therapy (CDT); CDT does not address proliferated fatty tissue but contributes to the reduction of edema and the prevention of the manifestation of lipo-lymphedema. The various components of CDT also contribute to reducing pain and hypersensitivity to pressure.
In most cases it is necessary to apply a lower level of compression (bandages and compression garments) due to pain and hypersensitivity in the affected areas. Compression garments generally have to be custom-made to the individuals’ measurements; however, some manufacturers offer lipedema garments in a number of standard sizes (4). If the use of compression garments is discontinued, edema will return.
Surgical treatment may be considered for patients with lipedema who do not respond to conservative treatment. Liposuction is currently the standard surgical treatment method; however, this procedure may cause bleeding and secondary damage to lymph vessels resulting in persistent swelling. New and more advanced techniques may reduce these risks; however, individuals considering this approach should ensure that the performing physician is experienced and follows internationally established guidelines.
Postoperatively, there is generally an increased tendency for swelling, thus CDT should be initiated or continued within a few days of the procedure.
In the presence of additional lymphedema (lipo-lymphedema) the treatment protocol for complete decongestive therapy corresponds with that for primary lymphedema. CDT shows good long-term results in lipo-lymphedema; however, affected individuals need to understand that although the lymphedemateous component responds well and generally relatively fast to CDT, the lipedema itself, i.e. the reduction of fatty tissue responds more slowly, and sometimes not at all. According to several authors, reduction of the excessive fatty tissue in lipedema is possible if compression garments are worn constantly.
Dear Lymphedema Blog Reader – if you like the contents on this website, please help to keep it going. A great amount of work and research is necessary to provide you with up-to-date information on this site. Your donation supports these efforts and associated administrative costs. Surplus funds will be donated to Lymphedema/Lipedema-related charitable endeavors. Please donate using the “Donate Now” button on the right upper hand of this page – Thank You!
Join Lymphedema Guru, a Facebook page solely dedicated to inform about all things related to lymphedema – news, support groups, treatment centers, and much more
(1) Herpertz, U. (1995) Das Lipödem. Lymphologie19, 1-11
(2) Földi, E., and Földi, M. (2006) Lipedema. In Földi’s Textbook ofLymphology (Földi, M., and Földi, E., eds) pp. 417-427, Elsevier GmbH,Munich,Germany
(3) Child AH, Gordon KD, Sharpe P, Brice G, Ostergaard P, Jeffery S, Mortimer PS. Lipedema: an inherited condition. Am J Med Genet A. 2010;152A:970–976. [PubMed]
(4) BRSENSATION.pdf
Additional Reading:
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3309375/


 Joachim Zuther, Lymphedema Specialist.
Joachim Zuther, Lymphedema Specialist.