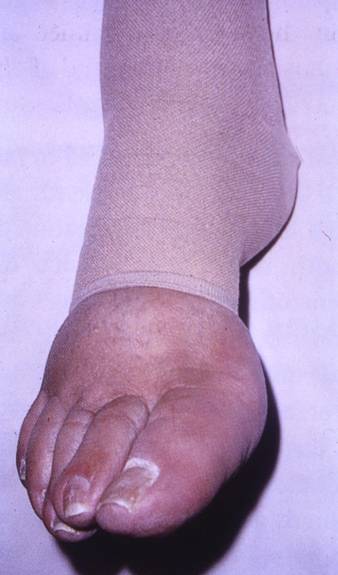
Skin and nail care play an essential role in both prevention of lymphedema in those patients at risk of developing this condition, and in the management of existing lymphedema. Current methods of cancer treatment lower the risk of developing lymphedema. However, if a patient had surgery involving the lymphatic system – a radical mastectomy for example – even many years ago, the risk for developing lymphedema will always be present, even if this patient never had any arm swelling.
Prevention is in the patients’ best interest and a great tool to avoid the onset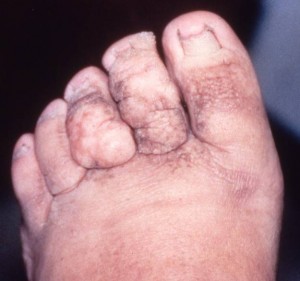 of lymphedema. The skin is the first line of defense against foreign invaders and is usually impermeable to bacteria and other pathogens. However, any defect in the skin such as burns, chafing, dryness, cuticle injury, cracks, cuts, splinters, insect bites and tattoo needles can present an entry site for pathogens or infectious agents and cause infection.
of lymphedema. The skin is the first line of defense against foreign invaders and is usually impermeable to bacteria and other pathogens. However, any defect in the skin such as burns, chafing, dryness, cuticle injury, cracks, cuts, splinters, insect bites and tattoo needles can present an entry site for pathogens or infectious agents and cause infection.
Patients who already have, or had lymphedema are susceptible to infections of the skin and nails. Lymphedematous tissues are saturated with protein-rich fluid, which serves as an ideal nutrient source for bacteria and other pathogens. Lymphedematous skin also tends to be dry and may become thickened and scaly, which increases the risk of skin cracks and fissures.
The process of inflammation may not only make lymphedema much worse by increasing the swelling, but can also develop into a serious medical crisis. The basic consideration in skin and nail care is therefore the prevention and control of infections, which includes proper cleansing and moisturizing techniques with the goal of maintaining the health and integrity of the skin.
Suitable ointments or lotions formulated for sensitive skin, radiation dermatitis and lymphedema should be applied before the application of lymphedema bandages while the patient is in the decongestive phase of the treatment. Once the limb is decongested and the patient wears compression garments, moisturizing ointments should be applied twice daily.
Ointments, as well as soaps or other skin cleansers used in lymphedema management, should have good moisturizing qualities, contain no fragrances, be hypo-allergenic and should be in either the neutral or acidic range of the pH scale (around pH 5). To identify possible allergic reactions to skin care products, they should be first tested on healthy skin before the initial application to areas affected by lymphedema. Skin care products often used by lymphedema patients include Eucerin, Lymphoderm, Lindi Skin products, Curel and Johnson&Johnson Baby Lotion.
Tight fitting compression sleeves or stockings, as well as materials used in compression bandaging may also cause skin irritation. Some patients may be allergic to a certain material used for compression therapy. This situation can be remedied by switching to other materials.
In mosquito infected areas it is necessary to apply insect repellents to the affected extremity (some moisturizers contain natural repellents) to avoid bites, which are a common cause for infections. To take proper care of mosquito bites and minor injuries, it is advisable to always carry an alcohol swab, antibacterial ointment and a band-aid.
 Tattoos in areas affected by lymphedema should be avoided; there are serious possible side effects associated with these procedures, such as infections, allergic reactions to the ink pigments and carriers, MRI complications, and blood borne diseases. In addition, new findings indicate that metal particles from tattoo needles have been found in lymph nodes (for more information see the links on the bottom).
Tattoos in areas affected by lymphedema should be avoided; there are serious possible side effects associated with these procedures, such as infections, allergic reactions to the ink pigments and carriers, MRI complications, and blood borne diseases. In addition, new findings indicate that metal particles from tattoo needles have been found in lymph nodes (for more information see the links on the bottom).
When caring for nails, it is important to keep the risk of infections to a minimum. Finger and toe nails should be kept short using clippers (no scissors), toenails should be cut straight across, and a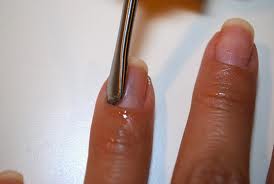 podiatrist should be consulted to treat and prevent ingrown toe nails. Cuticles on fingers and toes should not be cut but pushed back with a cuticle pusher.
podiatrist should be consulted to treat and prevent ingrown toe nails. Cuticles on fingers and toes should not be cut but pushed back with a cuticle pusher.
Bacteria between the natural and artificial nails are a common cause for infections; acrylic nails should be avoided.
Dear Lymphedema Blog Reader – if you like the contents on this website, please help to keep it going. A great amount of work and research is necessary to provide you with up-to-date information on this site. Your donation supports these efforts and associated administrative costs. Surplus funds will be donated to Lymphedema/Lipedema-related charitable endeavors. Please donate using the “Donate Now” button on the right upper hand of this page – Thank You!
Join Lymphedema Guru, a Facebook page solely dedicated to informing about all things related to lymphedema – news, support groups, treatment centers, and much more


 Joachim Zuther, Lymphedema Specialist.
Joachim Zuther, Lymphedema Specialist.